
FROM THE COUNCIL CHAIR AND CE
MESSAGE FROM THE CHAIR AND CE
Kia ora koutou
Thanks to everyone who completed their Annual Practicing Certificate application on time. We now have over 5000 pharmacists registered to practice in New Zealand from 1 April.
As you may have heard, the recent APC update included an unexpected defect affecting a specific area of functionality that caused all work addresses to be published, even for those practitioners who opted not to make this information public.
We recognise that privacy is closely connected to your personal safety and wellbeing, and if you were affected by this error, we sincerely apologise for the concern or distress this incident may have caused.
Pharmacy Council members recently approved the Council’s operating budget for FY2025/26. It will come as no surprise that costs are increasing across the board, as they are for everyone. We are working hard to manage every dollar effectively, but notifications keep increasing which means a corresponding increase in costs. If this trend continues, we may need to increase the discipline levy during the year to address costs.
In this newsletter you’ll also find an article about the purpose of the Assessment Centre and Council’s role in ensuring new pharmacists have the competency to practice safely and independently. The Council’s position is that we are open to different assessment options, but currently we are not prepared to lower safety or competence standards to increase the numbers of practicing pharmacists.
Finally, thanks to everyone who made a submission or attended a webinar on our recent discussion document to advance pharmacy practices. It was great to hear from so many people. We received some well-considered information that will help us prioritise our focus and actions for the coming years.
As we mentioned in the discussion document, this was not a formal consultation. Any regulatory tool changes that arise from this information will be communicated regularly and may have separate consultations (such as the consultation on proposed changes to the Recognised Equivalent and non-Recognised Equivalent Qualification Routes – see the article below). You’ll be hearing more in future newsletters.
Ngā mihi
Ming-chun Wu (Chair) and Michael Pead (Chief Executive)
IMPORTANT FOR YOU TO KNOW
APC APPLICATIONS
Thanks to everyone who got their Annual Practicing Certificate applications in before 31 March. We processed over 5000 applications, and a lot of people left their renewal to the very last minute, with 950 applications in the last 48 hours of the month!
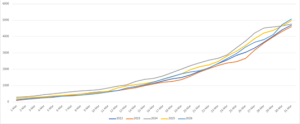
Cumulative applications over March
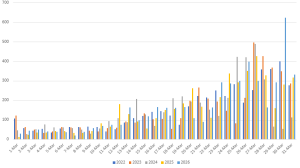
Applications received per day
What happens if I haven’t made an application by 31 March?
If we didn’t receive your application and fee by 31 March, on 1 April we changed your practising status to registered, inactive. Remember that you cannot legally practise in New Zealand as a pharmacist until you are issued with an APC (even if your role does not involve direct patient contact). If you still need to send in your application, please do it as soon as possible.
If for any reason you will not be practicing this year, you can transfer to inactive (non-practising) status or ask to be removed from the register. You can find more information and the registration status flowchart on our website.
From mid-April, we start a process called “register revision”, which helps to maintain the accuracy of the register. We send out reminders in May and November to anyone who has not put in an application and if a pharmacist has still not made contact by January 2027 their name will be removed from the register.
WORK ADDRESSES PUBLISHED ON THE PUBLIC REGISTER
Between 25 February and 30 March 2026, a technical issue with the Pharmacy Council’s website resulted in some pharmacists’ workplace address being visible on the public register on the website.
This occurred because a system change applied for the 2026/2027 APC year introduced a defect in the system used to process APC applications. The defect affected a specific area of functionality that caused all work addresses to be published, even for those practitioners who opted not to make this information public. This defect did not impact or disclose any other personal information or data field.
Once identified, the issue was addressed urgently and all work address details were immediately removed from Council’s website.
We recognise that privacy is closely connected to your personal safety and wellbeing. We sincerely apologise for the concern or distress this incident may cause.
We have treated this incident very seriously, including a full review of the error and how it occurred. We will take all steps necessary and reasonable to ensure that such an error does not occur in the future.
What information was involved
We can confirm that the information that may have been accidently visible is confined to your workplace address, as provided on your most recent APC application.
No other personal information, financial information, identity documents, email addresses, or account login details were involved.
What we are doing
We have:
- Removed workplace addresses from public access
- Undertaken an urgent review of our systems and processes
- Notified the Ministry of Health and the Minister’s office
- Notified the Office of the Privacy Commissioner
- Reviewed our systems to strengthen safeguards to prevent a similar incident in the future
Your privacy rights
Under the Privacy Act 2020, you have the right to make a complaint to the Office of the Privacy Commissioner if you remain concerned about this breach and/or are dissatisfied with our response.
Acknowledging the impact of this error
We acknowledge the seriousness of this incident and the impact it may have on your sense of safety, wellbeing and trust. We unreservedly apologise that this occurred and for any distress that it may have caused.
Council holds itself to the highest standards and we are committed to improving our systems and practices to better uphold privacy, safety, and trust.
If you have concerns about your safety
If you have concerns about the disclosure of your work address, you may wish to consider the following steps, to the extent they are relevant and appropriate to your individual circumstances:
- Review or update your safety plan, including plans that consider your whānau, tamariki, and wider support network.
- Contact New Zealand Police if you believe there is an immediate or increased risk to your safety (call 111 in an emergency).
- Let a trusted person know, such as an employer, colleague, whānau member, friend, kaumātua, or neighbour, so they can provide support or assistance.
- Keep a record of any concerning behaviour or contact, including dates and details.
- Seek culturally appropriate support from services that can provide guidance grounded in tikanga, Kaupapa Māori, or your cultural context.
Support services available in Aotearoa New Zealand
Confidential, free support is available nationwide, including culturally responsive services:
Emergency and General Support
- Police Emergency: 111
- Police non-emergency: 105
- Victim Support: 0800 842 846
Kaupapa Māori and Whānau-Centred Services
- Whānau Ora navigators – locally based support focused on whānau wellbeing
- Te Puna Aonui – Safer Whānau (via community providers)
- Māori Women’s Welfare League – local branch support and advocacy
- Te Rōpū Āwhina Wahine (where available)
Culturally Specific Services
- Shakti (Asian, African, Middle Eastern communities): 0800 742 584
- Women’s Refuge: 0800 733 843 (0800 REFUGE)
- Shine – Safer Homes in Aotearoa: 0508 744 633
These services can assist with safety planning, legal options, emotional support, and culturally grounded advocacy.
If you would like to discuss your circumstances or have specific safety concerns, please contact Michael Pead.
INCREASING NUMBERS AND COSTS FOR COMPLAINTS AND NOTIFICATIONS
The volume of complaints and notifications received by the Council continues to increase. During the 2025/26 practising year, case numbers rose steadily, from 21 in the first quarter to 27 in the second, then 32 in the third, before easing slightly to 31 in the final quarter.
The Council continues to manage most of these complaints at a local level, generally by taking an educative approach.
It remains the case, however, that a number of notifications still require full investigation by a Professional Conduct Committee, and potentially by the Health Practitioners Disciplinary Tribunal. These matters incur considerable costs, which the Pharmacy Council does not control, and we are continuing to see these costs increase.
If this trend continues, the Pharmacy Council may need to implement a disciplinary levy to cover the associated costs.
What is making costs increase?
Investigative processes, by their nature, take time and incur costs. These matters are considered by independent committees, whose work must be properly supported to ensure fair and well-reasoned outcomes. This includes legal advice and secretariat support to review information, manage processes, and ensure decisions are made carefully and lawfully. While this affects both timeliness and cost, these elements are essential to maintaining‑ fair, robust, and trustworthy processes.
Of the notifications that require a full investigation, we are seeing an increasing number of matters that are more complex in nature. These can require coordination with multiple agencies, involve repeated requests for additional information, include many witnesses, involve concerns spanning several years, and cover extensive documentation and multiple practitioners.
Managing this level of complexity takes time and resources, which can affect how quickly investigations progress and increases the overall cost of the process.
A small number of practitioners are increasing costs – why can’t they pay for the disciplinary process?
We often hear that it’s unfair for everyone to be covering the costs of pharmacists who do not meet the standards of competence and fitness to practice, and that those who do wrong should pay for the disciplinary process.
When a notification is received or a complaint is considered, our approach is that we proceed through a fair process.
Requiring a practitioner who is the subject of a notification or complaint to pay upfront for an initial inquiry by Council, a possible investigation by the PCC and any subsequent prosecution by the HPDT would be almost impossible to administer. Therefore, it is more equitable to spread the cost of compliance across all pharmacists.
What Council is doing to address costs
The Council continues to review how professional conduct committees are supported, with a focus on improving efficiency and identifying cost savings where possible. In doing so, we remain mindful of the importance of respecting committee independence and ensuring they are properly supported to carry out their vital role in protecting the public and upholding professional standards.
It’s critical that we continue to be notified of concerns to ensure public safety.
It is possible to reduce the costs associated with notifications and complaints when pharmacists engage proactively with the Council and are willing to reflect on and improve their practice. This helps to reduce the need for statutory action, which is where costs begin to increase significantly.
OUR ENGAGEMENT JOURNEY
PROPOSED CHANGES TO STREAMLINE OUR REGISTRATION PATHWAYS
 As mentioned in our recent Pharmacy Council discussion document, we have identified some immediate changes we can make to our registration pathways. We indicated we would move with urgency to help meet the workforce pressures the profession is having to deal with. These changes will help to streamline processes, making it as easy as possible for domestic and international pharmacists to register and practice safely in New Zealand, and for pharmacists to return to practice after time away from the profession.
As mentioned in our recent Pharmacy Council discussion document, we have identified some immediate changes we can make to our registration pathways. We indicated we would move with urgency to help meet the workforce pressures the profession is having to deal with. These changes will help to streamline processes, making it as easy as possible for domestic and international pharmacists to register and practice safely in New Zealand, and for pharmacists to return to practice after time away from the profession.
To complete these changes we need to update the secondary legislation – part of this process is a public consultation to make sure pharmacists agree with our proposals.
We are looking to make changes to the Pharmacy Council Scopes of Practice and Prescribed Qualifications Amendments Notice 2014. This gazette notice sets out the scopes of practice and qualification requirements.
You can read a copy of the consultation document on the consultations page of the Pharmacy Council website.
We are seeking feedback on four main areas:
- Amendments to the registration process for both the Recognised and non-Recognised Equivalent Qualification Routes.
- Removing reference to registration of Australian pharmacists via the Trans-Tasman Mutual Recognition Act 1997 and including a description of prescribed qualifications for United Kingdom Pharmacist Prescribers to register as a NZ Pharmacist Prescriber.
- Removing the requirement for pharmacists returning to practice after eight or more years to complete the Intern Training Programme and Assessment Centre.
- Minor corrections to the Gazette notice and editorial fixes to improve readability.
We invite responses from members of the pharmacy profession, the public and other interested individuals and organisations by 5pm on Monday 20 April 2026.
You can make a submission via this survey or by emailing your response to [email protected].
FEEDBACK ON THE DISCUSSION DOCUMENT
Thanks to everyone that made a submission and attended the webinars on our recent discussion document. As the regulator, we need to make sure we are set up for the changes needed to meet the challenges facing the sector.
The discussion document put forward some options on some key topics, and we asked the profession what’s important.
What you told us
We got useful information from the submissions, and we are working through the feedback. At a very high level, we heard that:
- There is broad but cautious support for endorsement frameworks, prescribing expansion, and regulating technicians, provided these are supported by clear governance, evidence, and safety frameworks
- There is widespread concern about pharmacist shortages, driven by poor remuneration, burnout, workload, and limited career pathways. Retention, not just faster registration or overseas recruitment, is seen as the most important factor to achieving workforce sustainability
- The Pharmacy Council must ensure that any changes or innovations include patient safety, evidence-based practice, risk assessment, and accountability as non‑negotiable requirements.
Next steps
While we received much feedback that we can use to shape our work priorities, there is also valuable information that we will be sharing with other parts of the sector, such as the Ministry of Health, Health NZ, education providers, and the professional organisations.
We are currently working through all the responses and will share the submissions and responses on our website. We’ll also keep you informed of how this information is shaping our work programme.
KEEPING YOU UP TO DATE
ABOUT THE ASSESSMENT CENTRE
 Last year, 153 people successfully passed the November 2025 Assessment Centre for intern pharmacists, which means they were eligible to register in the pharmacist scope of practice.
Last year, 153 people successfully passed the November 2025 Assessment Centre for intern pharmacists, which means they were eligible to register in the pharmacist scope of practice.
The Assessment Centre is the culmination of many years of work for intern pharmacists who have completed their degree and the intern training programme. It allows interns to demonstrate how the skills and competencies they have gained through their studies translate into safe clinical practice.
The pass rate for this Assessment Centre was 66%. Interns who did not pass may be able to sit the next Assessment Centre in May 2026.
What is the Assessment Centre, and why is it important?
The Assessment Centre is the final check that interns face to demonstrate they have the minimal level of skills, knowledge, and competencies needed to practice safely and autonomously as a pharmacist.
The Pharmacy Council Assessment Centre is an Objective Structured Clinical Examination (OSCE). This is a common and internationally valued way of assessing clinical competence for health professionals’ registration.
In the Assessment Centre, interns complete a series of timed clinical cases in a circuit. Each station has a trained examiner who assesses each intern’s clinical knowledge, communication skills, professionalism, and patient rapport against a standardised scoring sheet.
The Pharmacy Council and the Pharmaceutical Society of New Zealand work closely together to create an assessment that mirrors real-life clinical scenarios encountered in everyday practice. All cases are developed, reviewed, and assessed by practising pharmacists.
It is important that the assessment is not seen as an exam, but rather the fairest and most practical way to assess a group of interns at the same time on whether they are able to practice unsupervised. The cases are intended to be “real” examples of what pharmacists encounter, allowing interns to demonstrate that they can manage safely and independently.
Every year, the Pharmacy Council gets an external review of the examination to be confident of its integrity. The November 2025 exam has been confirmed to be psychometrically robust and in line with previous exams.
Are you concerned when the pass rate is lower than other years?
Pass rates can change year on year because interns are awarded a pass or fail result, and the total results are not scaled across the cohort.
This gives the public assurance that every intern who passes the Assessment Centre and registers as a pharmacist has the minimal skills and competencies needed to do the role independently.
Artificially improving pass rates by lowering standards below the level expected of a minimally competent practitioner will provide no benefit to pharmacists or the public.
Are there other ways to assess competency?
There are many ways to assess whether interns have the skills and competencies needed to take the next step, and we are open to supporting any assessment that results in safe practice.
Workplace assessments are often used as an example of an alternative assessment and may be something we move to in future if the sector prefers. Another option is to extend the supervision period or implement a “junior pharmacist” scope with restricted practice.
However, as interns currently move directly into unsupervised practice when they register in the pharmacist scope of practice, the Assessment Centre remains the fairest and most equitable way to independently assess whether an intern has the minimal competency needed to practice safely and autonomously.
CHILD PROTECTION TRAINING
It is critical that health practitioners who work with children are aware of possible signs of abuse and neglect, different types of abuse, and steps they are expected to take when they have concerns, including how to manage crisis situations and the importance of reporting and sharing information to support child safety.
The health system and its workforce have legislative and professional obligations regarding child protection, and training can improve awareness and practise.
In cases of suspected child abuse and neglect, there are processes that health practitioners are required to take which are set out in a Memorandum of Understanding between Health New Zealand, Oranga Tamariki, and the New Zealand Police. This includes expectations on health practitioners to notify Oranga Tamariki of all cases of suspected child abuse and neglect, and processes when infants, children, and young people are admitted to hospital following suspected or confirmed abuse or neglect.
The health sector is funded to implement this guidance through the Violence Intervention Programme (VIP). The VIP aims to reduce and prevent the health impacts of violence and abuse through early identification, assessment, and referral of people who would benefit from specialist supports or health services.
Health New Zealand has regional VIP co-ordinators and national training facilitators who deliver training and provide information about relevant services and referral processes to health professionals. Training and resources are available, and you can find out more on the Ministry of Health’s website.

